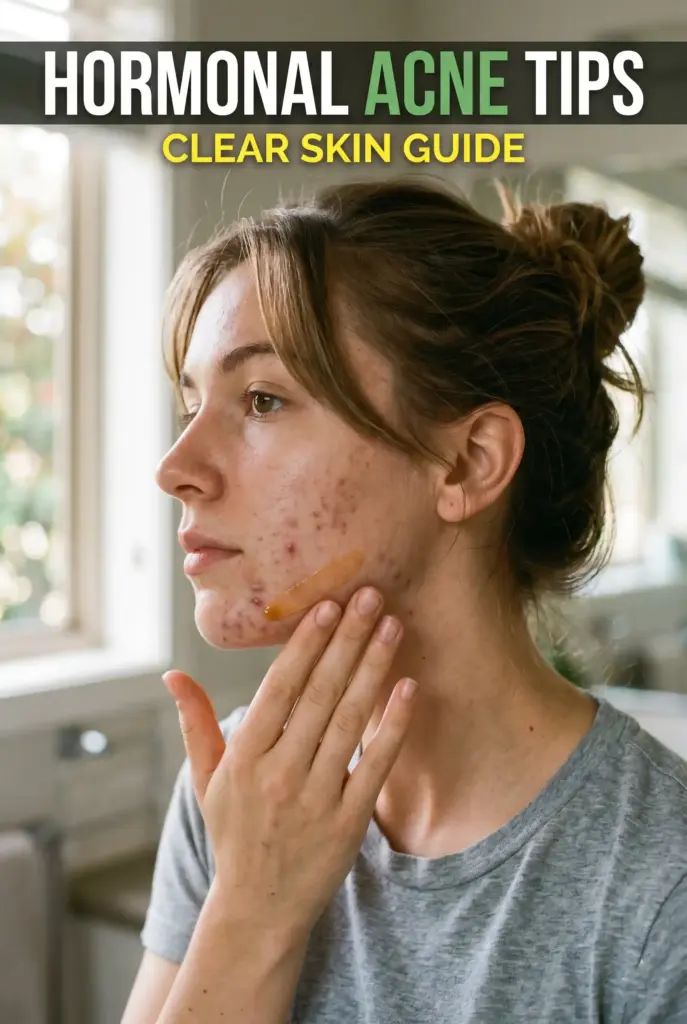
Hormonal acne is one of the most frustrating skin conditions because it behaves differently from teenage or surface-level acne and refuses to respond to the same treatments. It tends to appear in predictable locations — the lower face, jaw, chin, and sometimes the neck and chest — in a cyclical pattern that worsens in the days before menstruation, at ovulation, or during periods of high stress. It produces deep, cystic, painful spots that sit below the surface for days before coming to a head, and leaves behind dark marks that take weeks to fade.
Standard acne advice — stronger cleansers, more benzoyl peroxide, more exfoliation — does little for hormonal acne because it treats the surface while the cause is internal. Effective hormonal acne management addresses the hormonal drivers directly, supports the skin barrier rather than stripping it, and uses targeted treatments that match the specific inflammatory pattern of androgen-driven breakouts.
| Did You Know? Hormonal acne is driven primarily by androgens — testosterone and its more potent derivative DHT — which stimulate sebaceous glands to produce more sebum. In women, androgen levels naturally spike in the days before menstruation, at ovulation, during high-stress periods (cortisol converts to androgen), and in conditions including PCOS. This explains the predictable timing and location of hormonal acne — the jawline, chin, and lower face have the highest density of androgen-receptor-rich sebaceous glands. |
Internal Tip 1: Balance Blood Sugar to Reduce Androgen Production
Blood sugar dysregulation is one of the most significant and most overlooked drivers of hormonal acne. When blood sugar spikes from refined carbohydrates and sugar, insulin rises sharply — and elevated insulin directly stimulates the ovaries and adrenal glands to produce more androgens. More androgens mean more sebum production, more blocked pores, and more hormonal acne. Eating protein and fat at every meal before carbohydrates, choosing complex over refined carbohydrates, reducing added sugar, and never eating carbohydrates alone without a protein or fat to buffer the glucose response all stabilise insulin in ways that directly reduce the androgen production driving hormonal breakouts. Most people who clean up their blood sugar management notice reduced jawline and chin breakouts within two to three menstrual cycles.
Internal Tip 2: Support Liver Health for Better Hormone Clearance
The liver is responsible for metabolising and clearing used hormones including oestrogen and testosterone from the body. When liver function is sluggish — from alcohol, processed food, inadequate cruciferous vegetables, or chronic stress — hormones recirculate rather than being excreted, contributing to the hormonal excess that drives acne. Supporting liver detoxification directly improves hormonal balance and reduces hormonal acne over time. Eat cruciferous vegetables daily — broccoli, kale, cauliflower, Brussels sprouts — for their DIM content that specifically supports oestrogen detoxification. Start every morning with warm lemon water. Reduce alcohol significantly — it is one of the most liver-congesting and hormone-disrupting substances women regularly consume.
Internal Tip 3: Manage Cortisol Actively
Cortisol — the primary stress hormone — directly converts to androgens through the same biochemical pathway, meaning that every period of high stress increases the androgen load that drives hormonal acne. Women who notice that their breakouts worsen significantly during stressful periods are observing this cortisol-to-androgen pathway in action. Managing cortisol is therefore a direct acne management strategy: consistent sleep times, daily moderate exercise (avoiding very intense late-evening training that spikes cortisol), daily stress management practice, and ashwagandha supplementation (shown to reduce cortisol by up to 28% in clinical research) all reduce the stress-driven androgen production that triggers breakouts.
Internal Tip 4: Supplement With Spearmint Tea and Zinc
Two natural supplements have specific clinical evidence for hormonal acne. Spearmint tea consumed twice daily has been shown in randomised controlled trials to reduce free testosterone levels measurably in women over four to eight weeks — directly reducing the androgen stimulus driving hormonal sebum overproduction. Zinc at 30mg daily supports follicle repair, inhibits the conversion of testosterone to the more potent DHT (the direct acne-driving androgen), and reduces the inflammatory response that makes hormonal spots so painful and inflamed. Both interventions are most effective when maintained consistently for a full two to three menstrual cycles before assessing results.
Topical Tip 1: Use Niacinamide as Your Primary Treatment
Niacinamide — vitamin B3 — is the most targeted topical treatment for hormonal acne available without a prescription. It reduces sebum production by regulating the activity of sebaceous glands at the cellular level — directly addressing one of the primary surface manifestations of androgen excess. It reduces the post-acne pigmentation that hormonal acne leaves behind, calms the chronic low-grade skin inflammation that makes hormonal breakouts so red and swollen, and strengthens the skin barrier that over-treating with acids and benzoyl peroxide has likely already compromised. Apply a 5 to 10% niacinamide serum to the lower face every morning and evening after cleansing. Most people notice reduced oiliness and fewer new breakouts within three to four weeks.
Topical Tip 2: Never Over-Strip the Skin
The most common mistake in hormonal acne treatment is applying the same aggressive approach used for teenage acne — harsh cleansers, strong acids, frequent exfoliation — to skin that is already inflamed and barrier-compromised from hormonal fluctuations. Over-stripping triggers reactive sebum overproduction that worsens the hormonal acne cycle. Use a gentle, pH-balanced cleanser twice daily — nothing that leaves skin tight or dry. Exfoliate with a gentle BHA (salicylic acid 1 to 2%) just two times per week rather than daily. Keep the skin barrier intact and well-moisturised at all times — a healthy barrier responds to hormonal fluctuations significantly better than a compromised one.
Topical Tip 3: Targeted Spot Treatment for Active Cysts
For the deep, cystic spots characteristic of hormonal acne: apply a thin layer of plain aspirin paste (crush one uncoated aspirin tablet with a drop of water) directly to the cyst overnight. Aspirin is acetylsalicylic acid — it reduces the prostaglandin-driven inflammation inside the cyst directly, reducing size and pain significantly by morning. Alternatively, hydrocolloid patches placed over early-stage hormonal spots absorb the fluid from developing cysts, protect them from picking, and create a moist healing environment that resolves spots faster and with significantly less post-inflammatory pigmentation than untreated spots. Never pick, squeeze, or extract hormonal cysts — the deep inflammation spreads into surrounding tissue and guarantees the dark marks that are harder to treat than the original spot.
| Pro Tip: Track your breakouts against your menstrual cycle for two to three months — noting when new spots appear, where they are, and the day of your cycle. This mapping reveals whether your acne is truly hormonal (predictable pre-menstrual and ovulation patterns in the lower face) versus stress-driven (random timing, related to high-pressure periods) or dietary (appearing after specific foods or alcohol). The pattern tells you which internal interventions to prioritise. |
Hormonal acne is not a skincare problem alone — it is a systemic hormonal condition that requires a whole-body approach for genuine, lasting improvement. Stabilise blood sugar, support liver health, manage cortisol, and supplement strategically on the inside. Use a gentle barrier-supportive routine with niacinamide on the outside. Give this combined approach two to three full cycles and let the pattern of your skin — not the perfection of a single week — show you what genuine hormonal balance produces.